Common Myths About Robotic Joint Replacement Surgery – What Patients Should Really Know
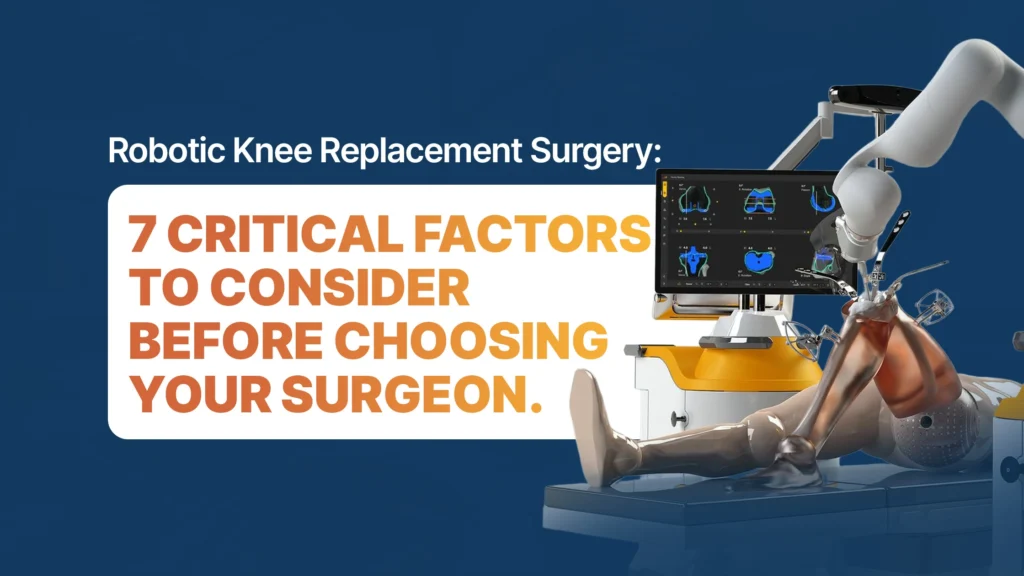
Common Myths About Robotic Joint Replacement Surgery – What Patients Should Really Know Robotic joint replacement surgery has gained significant attention in recent years. Many patients today specifically ask whether their knee or hip replacement will be performed using robotic assistance. While robotic technology has improved surgical precision and planning, there are still several misconceptions surrounding the procedure. According to Dr. Abhishek Bhalotia, understanding the difference between myths and facts helps patients make informed decisions about their treatment. Below are some of the most common myths about robotic joint replacement surgery and the facts patients should know. Myth 1: The Robot Performs the Entire Surgery One of the most common misunderstandings is that the robot independently performs the surgery. In reality: The surgery is performed by the orthopaedic surgeon. The robotic system assists with surgical planning and precision. The surgeon controls every step of the procedure. The robot functions as a guidance tool, helping the surgeon position implants more accurately based on pre-operative planning. Myth 2: Robotic Surgery Guarantees Perfect Results While robotic technology improves accuracy, it does not guarantee identical outcomes for every patient. Joint replacement outcomes depend on several factors, including: Severity of arthritis Bone quality Soft tissue balance Patient health and rehabilitation Robotic assistance can enhance precision, but surgical expertise and patient recovery still play a crucial role. Myth 3: Robotic Surgery Means No Pain After Surgery Some patients assume that robotic surgery eliminates post-operative discomfort completely. However: Mild to moderate pain is expected after any surgical procedure. Pain typically improves gradually during the recovery period. Structured physiotherapy and rehabilitation help manage discomfort and restore mobility. Robotic surgery may support better alignment and soft tissue balance, which can contribute to smoother recovery, but it does not eliminate all post-operative pain. Myth 4: Every Patient Must Have Robotic Joint Replacement Another misconception is that robotic surgery is necessary for all joint replacement cases. In practice: Some patients benefit from robotic planning due to complex anatomy or alignment issues. In other cases, conventional techniques may achieve excellent results. The choice of technique should be based on the patient’s specific condition rather than marketing trends. Myth 5: Recovery Is Instant with Robotic Surgery Although modern techniques allow early mobilisation, recovery still requires time and rehabilitation. Patients usually experience: Early walking within a short time after surgery Gradual improvement in strength and balance Several weeks of physiotherapy for optimal recovery Even with advanced technology, recovery remains a step-by-step process. Why Robotic Technology Is Still Valuable Despite the myths, robotic systems offer meaningful advantages when used appropriately. These may include: Improved implant positioning accuracy Better surgical planning based on imaging Greater precision during bone preparation Potential improvement in joint alignment When combined with surgical expertise, robotic assistance can contribute to consistent and predictable outcomes. What Patients Should Focus on Instead Rather than focusing only on whether surgery is robotic, patients should evaluate: Surgeon’s experience in joint replacement Clear explanation of treatment options Realistic expectations regarding recovery Availability of structured physiotherapy and follow-up care A successful joint replacement is the result of good planning, careful surgical execution, and active patient participation during rehabilitation. Final Thoughts Robotic joint replacement surgery represents an important advancement in orthopaedic care, but it should be understood realistically rather than through exaggerated claims. As Dr. Abhishek Bhalotia emphasises, robotic technology is a valuable tool that supports surgical precision, but the ultimate success of joint replacement still depends on thoughtful surgical planning, proper technique, and patient commitment to recovery. When patients separate myths from facts, they can approach joint replacement surgery with greater confidence and clarity.